‘It’s borderline criminal’: Spokane couple gets $2.2K surprise medical bill
SPOKANE, Wash. — Even with health insurance, patients can still get hit with an unexpected medical bill in Washington state.
The Washington state legislature passed a law to stop a loophole that allows surprise medical bills to happen, but the loophole doesn’t close until 2020.
A Spokane couple spoke to KREM 2 about how this happened to them, even after they checked with their insurance to make sure everything was covered.
Monte and Kristy Jones received an unexpected bill after Monte had surgery for a bulging disk. Before they scheduled surgery, they made certain that — after a co-pay — insurance would cover the cost.
“They said, ‘You’re approved, go ahead and schedule it,’ and that’s what we did,” Monte said.
Kristy checked as well, adding, “Even at the pre-op appointment I even asked again, our insurance there’s no problem with our insurance we’re covered. And they said yes.”
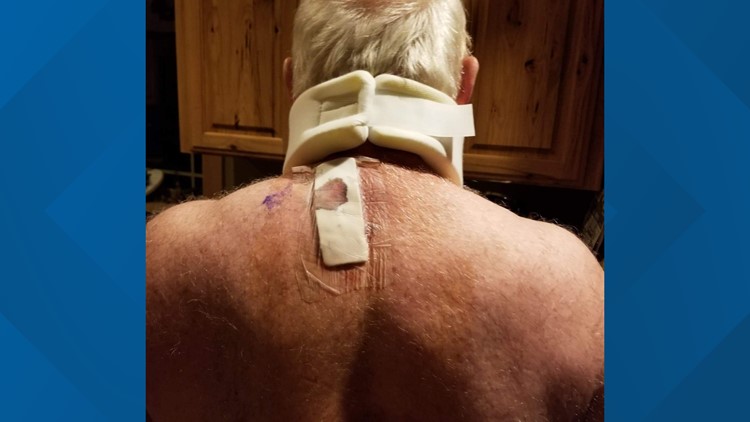
“And they were out of our network and so it’s $2,250. And (the bill said) that our insurance paid $960.37 of that,” said Kristy.
That’s when they learned about surprise or “balance billing.”
Statistically, 60 percent of people have gotten one of these types of bills. When patients go to a hospital they may be treated by a doctor who accepts their insurance. But if somebody comes in to help who isn’t in-network, the patient is likely to end up with a separate, surprise bill for a balance above and beyond what insurance agreed to pay that provider. That’s when patients get a bill for the balance.
“We have a past due amount now,” said Kristy, “And so we’re worried, well, we don’t want it to go to collections.”
“I think it’s completely wrong. To me it’s borderline criminal,” added Monte.
Washington Insurance Commissioner Mike Kreidler agrees. He’s heard patient complaints about surprise billing for decades, including two this year where consumers were hit with unexpected bills of nearly $100,000.
